The pathway of care for 3-6 month olds is different from the 0-12 week olds. This is because it can be harder to facilitate an infant of this age group to change how they feed. Their compensatory movement patterns are more established and their newborn feeding reflexes are no longer present for us to work with.
A baby who has a tongue tie will have had to adapt to this structural restriction from before they were born. They will therefore have developed compensation strategies to feed, which in turn causes tension patterns in their body; for example, you may have noticed they turn their head one way more than the other or they find tummy time hard.
Helping your baby to transition to a normal feeding pattern, using the muscles in the way they were intended, and building up sufficient stamina, is going to take time and assistance from you. We therefore need to show you how to do this, and your baby will find this process following surgery much easier if they are prepared ahead of time.
This means they will benefit from having feeding support/feeding therapy appointment(s) ahead of surgery to improve their chances of transitioning their feeding to normal movement patterns after surgery and achieve the best outcome.
The initial appointment will be a consultation to assess if there are tethered oral tissues (Tongue, Lip or Buccal ties) and assess your child’s feeding. A recommended treatment plan will be discussed with you.

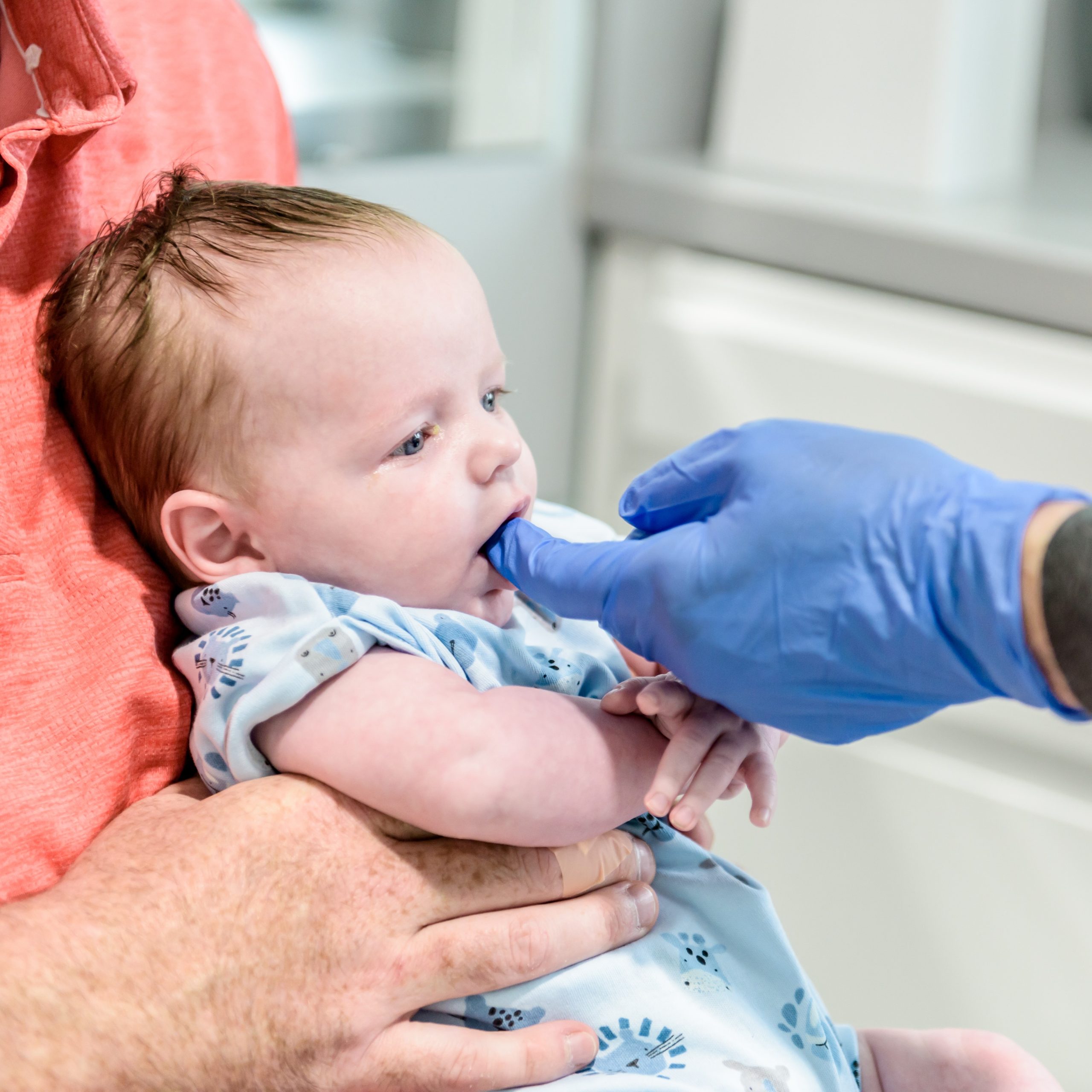
One of our feeding specialists, International Board Certified Lactation Consultants (IBCLC), will assess how your baby is feeding to review how their function is. They will be looking at whether your baby is moving their tongue to create suction to extract milk. Alternatively, they may be using tongue or lip compression, tongue thrusting or jaw dropping to achieve milk transfer. They will also observe how your baby paces themselves when feeding. They will assess latch and position and suggest changes to optimise this if you are breastfeeding. If you are bottle feeding they may suggest a change in bottle type and/or flow rate.
We will examine your baby and then discuss the findings of both this and the feeding assessment. A recommended treatment plan will be drawn up to best prepare for surgery, if this is required. Surgery will be performed on a different day.
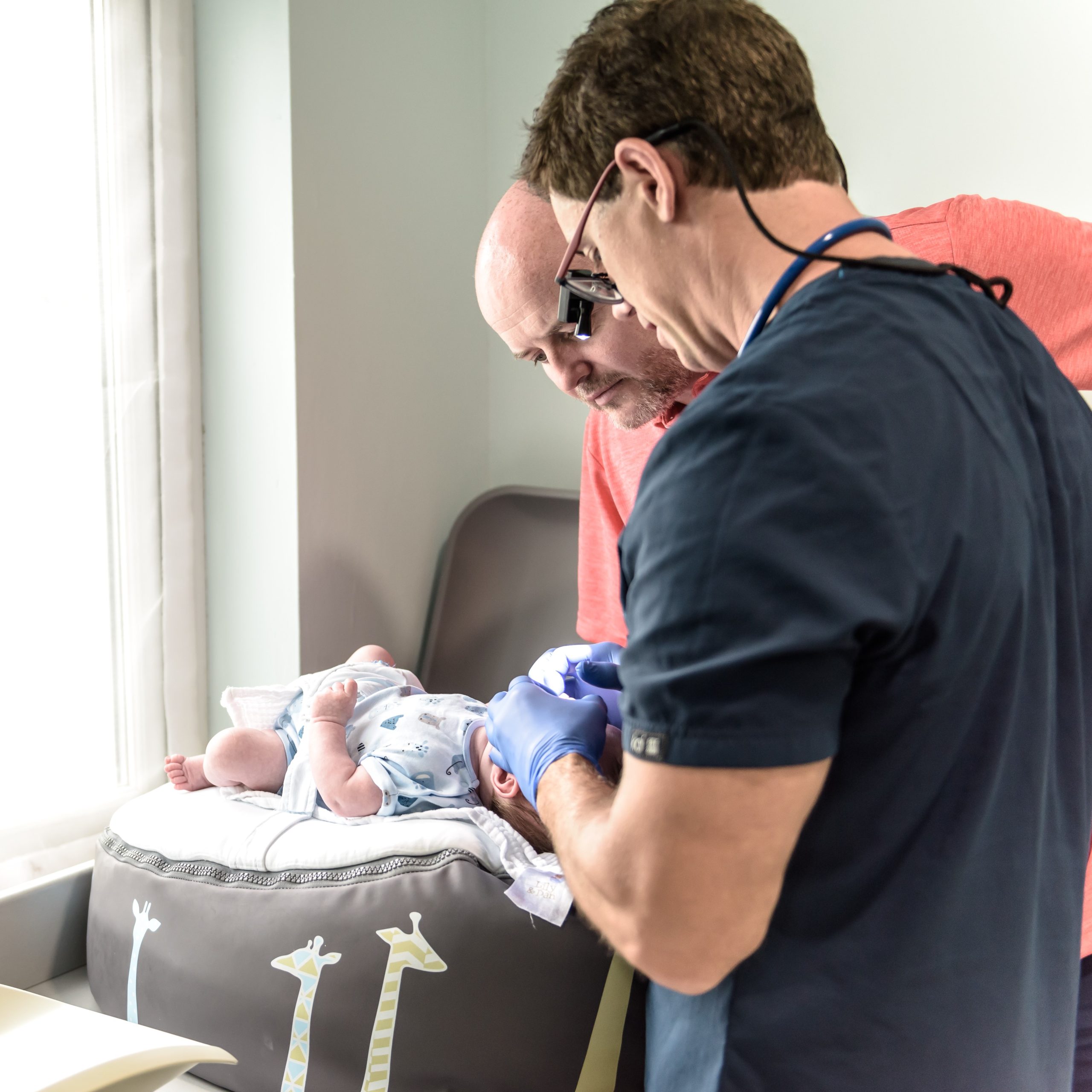
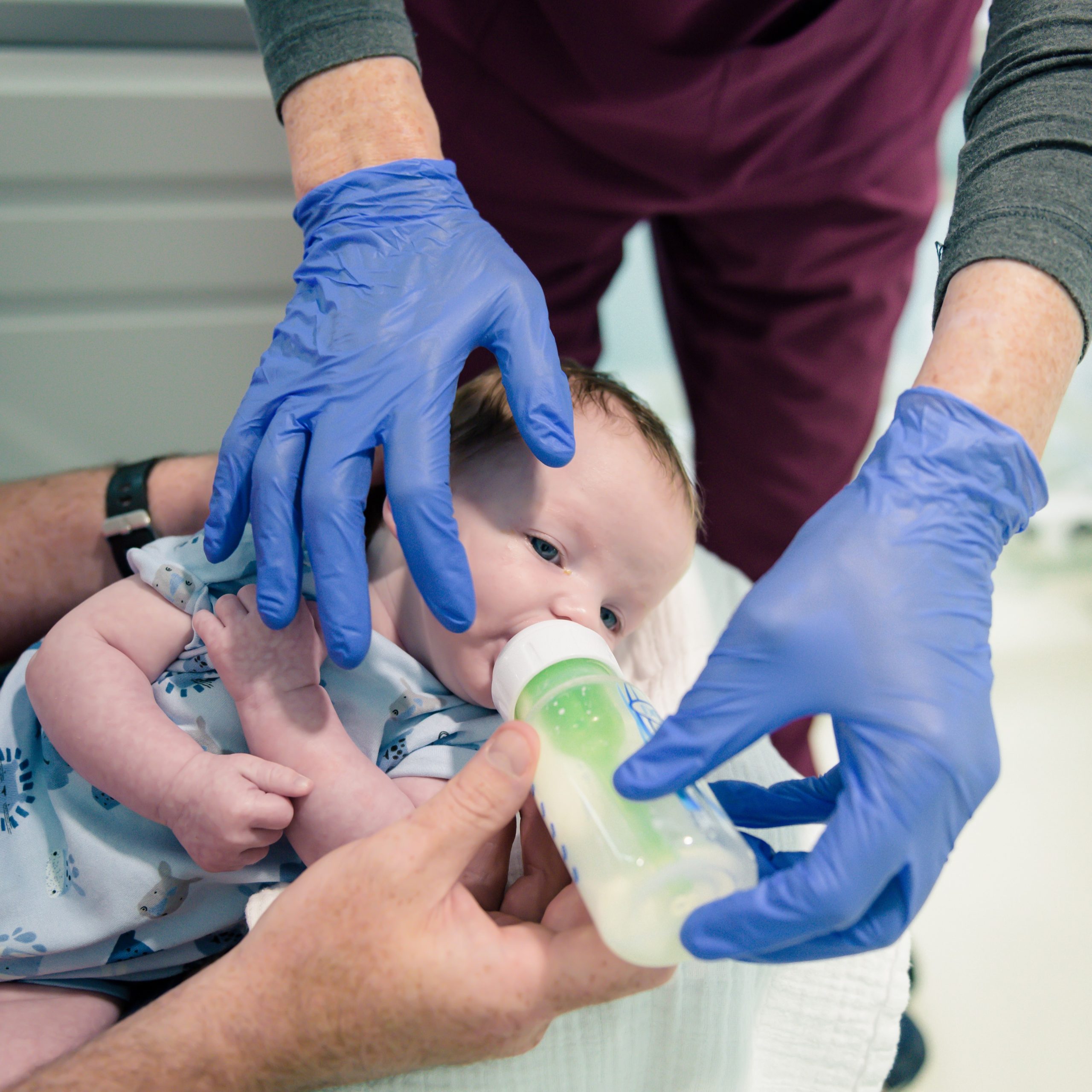
Feeding support appointments can be offered pre-surgery to help you and your baby prepare so that you achieve the best surgical outcome.
You will also be offered feeding support appointment(s) in the days following surgery. Achieving an optimal outcome from treatment and correcting dysfunctional feeding is a process which takes time and often adjustment to treatment and advise depending on how your baby is progressing.
Feeding therapy is an appointment with a Physiotherapist who has specialist training in infant feeding. This is often recommended if a baby has a higher degree of oral dysfunction or has added issues such as feeding aversions.
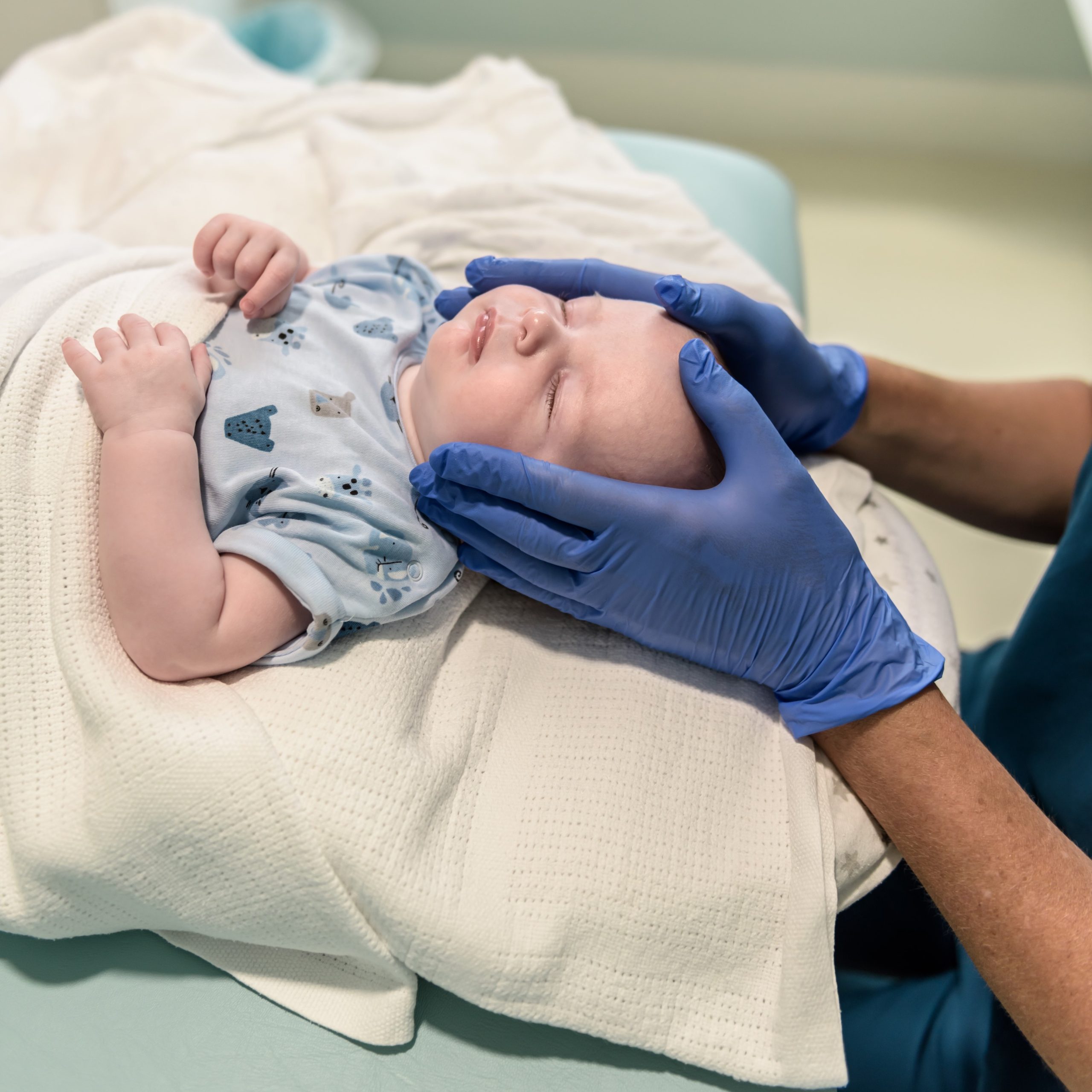
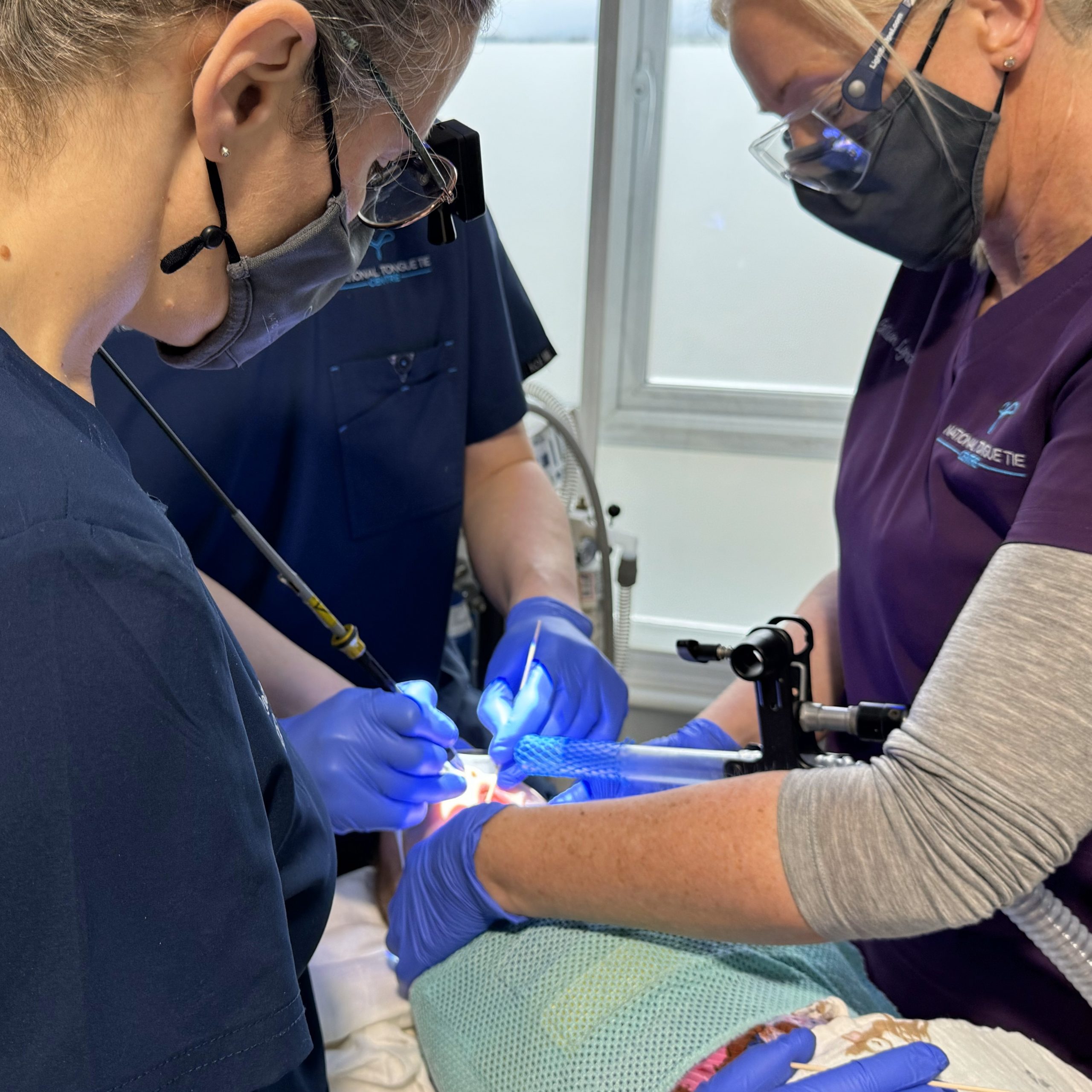
This step is the surgery for the Tongue/Lip/Buccal Tie(s).
For this, we use conscious sedation. This means that although your child will be breathing for themselves they will be unaware of what is going on and have no memory of the procedure. They are kept comfortable by numbing the base of the tongue using local anaesthetic. Throughout the procedure and for a while after, we will have them monitored using an ICU-grade monitoring system.
As your child is conscious during surgery we can elicit tongue movements and they have normal tone in the muscles, so we can more precisely gauge how much fibrous tissue needs to be released for optimal function whilst creating minimal inflammation during the healing process. Both doctor and physiotherapist work together in surgery ensuring all tension has been released under the tongue. This is what differentiates a functional frenuloplasty from a tongue tie release under general anaesthetic as with this method the patient is fully unconscious and muscles flaccid.
The surgical site is held together using absorbable sutures so that there is no need for any active wound management post-operatively, minimising inflammation and post-operative discomfort.
The work you will have been doing ahead of surgery is continued and monitored so that we obtain optimal healing of the surgical suture line, correct dysfunction and achieve habituation of normal movement patterns. The number of appointments depends upon the response to treatment.
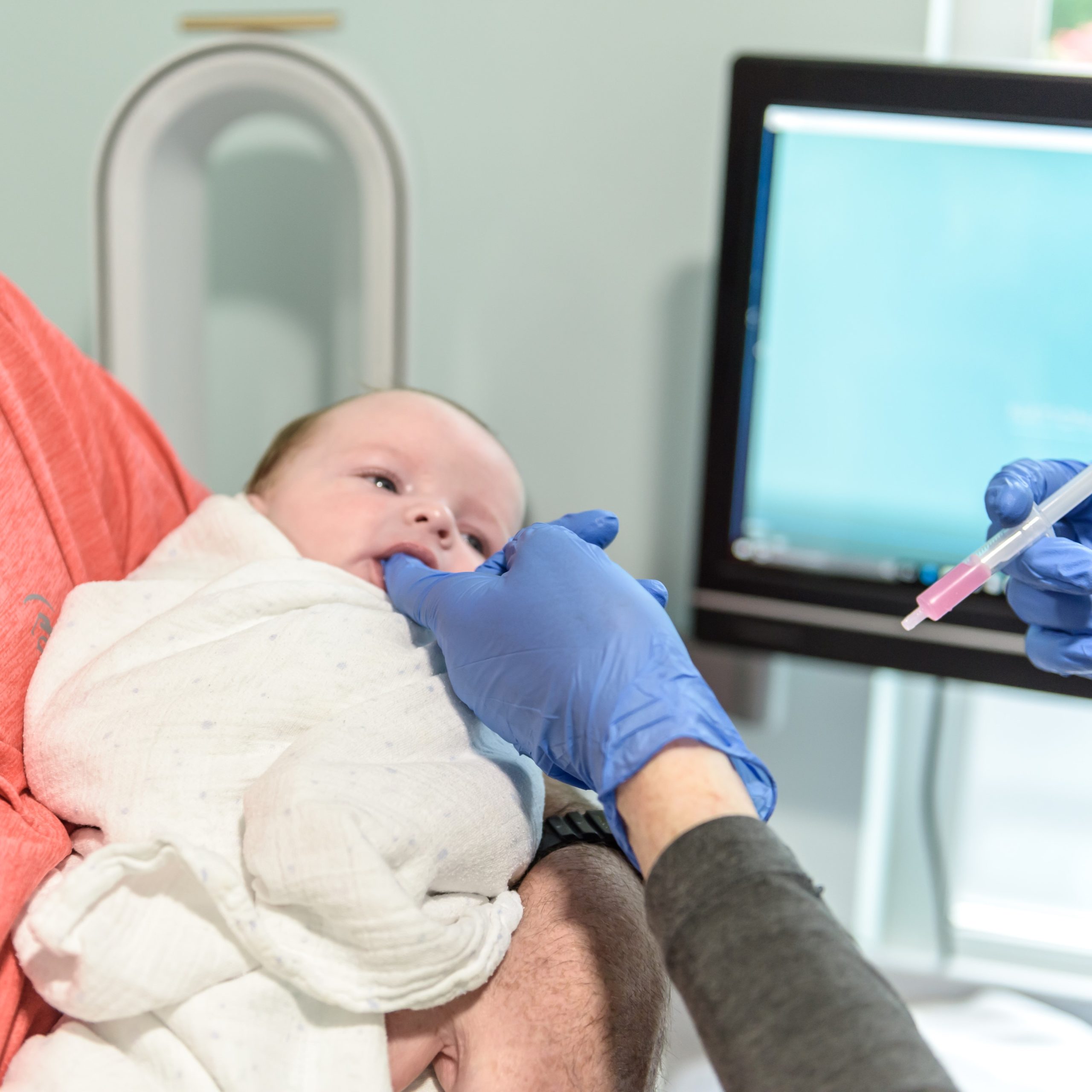

We will arrange an appointment with a Doctor approximately 8 weeks post surgery to check that the sutures have been fully absorbed and to check progress.
Copyright – National Tongue Tie Centre 2024